
MOLLUSCUM CONTAGIOSUM
Molluscum Contagiosum is a viral skin condition that can affect all ages, although it most commonly affects the pediatric population. This condition causes firm, painless,

ATOPIC DERMATITIS (ECZEMA)
Atopic dermatitis, most commonly known as eczema, is an inflammatory skin condition that is caused by a disruption of the skin’s natural barrier. Atopic Dermatitis

DRY SKIN
Dry skin, also known as xerosis, is a condition in which the skin barrier becomes irritated, which can lead to flaking and cracking of the

WARTS
Warts, also known as verruca vulgaris, are a common skin condition among children. Warts are raised or flat skin colored, white, or greyish bumps that

BIRTHMARKS
Birthmarks are markings on the skin that occurred while in utero that are now presented on the skin post birth. These markings can also develop

DIAPER RASH
Diaper rash, also called diaper dermatitis, is a skin condition that affects infants and toddlers who wear diapers. The sensitive skin in the diaper area

SEBORRHEIC DERMATITIS/CRADLE CAP
Seborrheic dermatitis, also known as cradle cap in infants, is an inflammatory skin condition that causes redness and yellowish, waxy, greasy looking scales on the
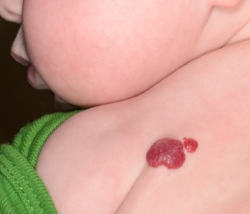
HEMANGIOMAS
Hemangiomas are a type of vascular birthmark that appear right after birth or within the first few weeks of an infant’s life. They appear as


